Abstract
Summary: We report the case of a 74-year-old woman with a complex indirect (Barrow D) carotid cavernous sinus fistula. The patient was treated incrementally and finally cured by a rarely reported bilateral retrograde direct transvenous approach via the superior ophthalmic vein. The treatment of the complex carotid cavernous fistula with multiple bilateral fistula points showed additional complexity due to a partially thrombosed left superior ophthalmic vein, which required a combined microsurgical and endovascular treatment, showing that treatment can be achieved, if necessary, by catheterization of a thrombosed orbital vein.
According to Barrow et al (1), carotid cavernous fistulae (CCF) are classified into direct (type A) and indirect (types B–D) types. Direct CCF are high flow shunts between the cavernous portion of the internal carotid artery and the cavernous sinus and are usually caused by traumatic laceration of the internal carotid artery or rupture of an intracavernous carotid aneurysm (2). Indirect CCF are dural fistulae between the cavernous sinus and extradural branches of the internal carotid artery, the external carotid artery, or both. Type B are fistulae between meningeal branches of the internal carotid artery and the cavernous sinus. Type C are dural shunts between meningeal branches of the external carotid artery and the cavernous sinus. Type D are fistulae between meningeal branches of both the internal carotid artery and external carotid artery and the cavernous sinus. For Barrow type B–D indirect CCF, transvenous embolization with GDCs has been widely accepted as the treatment of choice (3, 4). Transarterial embolization can markedly decrease a large amount of the shunt volume, but it is not likely to result in complete elimination. Therefore, its use is limited to type C CCF (5) or as additional treatment in cases of type D CCF.
In this report, we describe the treatment of a type D CCF, focusing on the combined microsurgical and endovascular treatment via a superior ophthalmic vein (SOV) approach. The SOV route was first described in 1969 (6) and has been subsequently described by several authors (3, 7–10). To our knowledge, a surgical approach through a thrombosed SOV has been published in only two cases (8).
Case Report
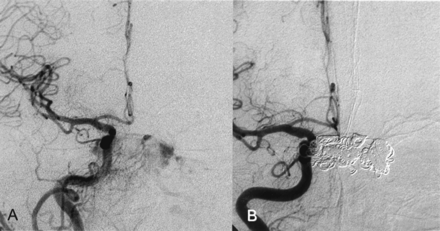
Two months before admission, a 74-year-old woman developed diplopia, exophthalmus on the left side, scotomas, left visual blur, and left conjunctival injection. MR imaging, MR angiography, CT, and duplex sonography revealed a CCF. At the time of admission, the patient had exophthalmus on the left, visual disturbance, diplopia, bilateral abducens nerve palsy, and left oculomotor nerve palsy. Angiography revealed a Barrow type D CCF with bilateral fistulae of the cavernous sinus fed by multiple meningeal branches of the external carotid artery on both sides, by the anterior meningeal branch of the left vertebral artery, and by the internal carotid artery on the left side (Figs 1 and 2). The CCF drained from the cavernous sinus into the right SOV, the left pterygoid venous plexus, the left inferior petrosal sinus, and via cortical veins into the straight sinus and the lateral sinuses on both sides. The right inferior petrosal sinus could not be detected. In contrast to the initial MR angiography performed 4 weeks earlier, the angiography showed the left SOV being thrombosed.
Right CCA.
A, Before treatment.
B, After successful CCF treatment.
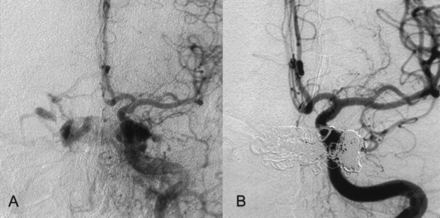
Left CCA.
A, Before treatment.
B, After successful CCF treatment.
The treatment required three sessions. During the first session, the embolization was performed immediately after diagnostic angiography by a transfemoral transvenous approach through the left inferior petrosal sinus into the cavernous sinus. Although 16 GDCs (Boston Scientific, Fremont, CA) were delivered into the left cavernous sinus and into the intercavernous part by using attenuated packing, the treatment remained incomplete with persistent multiple fistulae.
During the second session 4 days later, passing a microcatheter via the left inferior petrosal sinus was impossible because of aplasia or occlusion. A transfemoral transvenous approach via the facial vein into the left SOV was impossible because of a local thrombosis at the superior external angle. After a transfemoral transvenous approach via the right SOV, the position of the microcatheter was unstable and only two GDCs could be placed into the intercavernous part of the cavernous sinus. The CCF was not eliminated. Therefore, an attempt was made by using a transarterial approach with occlusion of meningeal branches of the external carotid artery (middle meningeal artery, accessory meningeal artery, and meningeal branches of the internal maxillary artery) on both sides with Ethibloc (Johnson + Johnson, Brussels, Belgium), resulting in flow reduction.
Because the neurologic deficits of the patient did not improve, the patient was treated 2 weeks later in a third session while under general anesthesia. First, a new attempt at a transvenous approach, via both inferior petrosal sinuses and facial vein into the SOV on both sides, failed. Therefore, a microsurgical approach in the catheter laboratory, with exposure of the SOV on the right side, was chosen. A 2-cm skin incision in the upper eyelid was performed, and the orbital septum was opened by the neurosurgeon. Microsurgical preparation of the orbital fat and exposure of the dilated SOV were performed. The vein was secured with a vessel loop and intraoperative micro-Doppler imaging showed high arterial flow. The vein was punctured with a 0.018-gauge cannula (Braun, Melsungen, Germany) and temporarily fixed with a 4.0 suture. This was used as a sheath for introducing a FasTracker18 (Boston Scientific, Cedex, France) with a 0.014-in TransendEx microguidewire (Boston Scientific, Fremont, CA). After the embolization, the cannula was removed and the opening in the SOV was closed by using an 8.0 suture. Finally, the skin was closed with interrupted 6.0 nylon sutures.
However, the CCF could not be occluded despite the deployment of another nine GDCs. Therefore, a second microsurgical approach via the thrombosed left SOV was attempted. The surgical procedure was performed as on the contralateral side; however, the thrombosed SOV was not easy to detect and prepare. Intraoperative micro-Doppler imaging confirmed the thrombosis of the left SOV. The vein was punctured nevertheless, and under fluoroscopy, a microguidewire could be pushed forward through the soft thrombus. This allowed intracavernous placement of a two-tip Tracker 18, with successful endovascular occlusion of the CCF being achieved after an additional deployment of eight GDCs (Figs 1 and 2).
In total, the Barrow type D CCF was cured in three sessions with 35 GDCs (23 standard coils and 12 vortex coils; Boston Scientific, Fremont, CA) and with Ethibloc.
The postprocedural course was uneventful. Ten days after the last embolization, the patient was discharged with marked improvement of the ophthalmologic symptoms. Six weeks later, the patient showed almost complete recovery, with slight residual ptosis on the left side and a slight bilateral disturbance of eye motility without nerve palsy. The visual acuity had improved from 0.1 to 0.5 on the left side and from 0.4 to 0.8 on the right. Results of duplex sonography were normal, showing no arteriovenous shunts.
Discussion
We report the successful occlusion of a complicated bilateral indirect CCF (Barrow type D) by an extremely rare bilateral SOV approach performed in one session. Additional venous thrombosis of the left distal SOV was expected to render catheterization of the fistula impossible, but the thrombosed segment was easily passed with the catheter without complications. Although the potential surgical complications of the SOV approach are hemorrhage, damage to the trochlea or other orbital structures, and infections (8), the surgical SOV approach is a safe, direct, and efficient way to access and occlude the cavernous sinus (8–10). Despite the risk of the approach itself, the main complication associated with transvenous embolization is over-packing of the cavernous sinus resulting in nerve palsies, dural dissections, or penetrations (5). Therefore, the less risky transfemoral transvenous approach was preferred initially.
Indirect CCF are rarely life threatening. Because of the high rate of spontaneous regression between 9.4% and 50%, in most cases, a “wait and see” strategy may be appropriate (1, 4, 7, 8). In cases of rapidly deteriorating ocular symptoms and/or cortical venous drainage, urgent interventional therapy is indicated (4). These criteria were present in our patient.
Transfemoral transvenous embolization has become the treatment of choice, especially for indirect (Barrow type B–D) CCF. Alternative or additional treatment strategies are transarterial embolization, a combined surgical and endovascular SOV approach, and the surgical exposure of the cavernous sinus to perform direct embolization (11). Our case shows that a complex CCF requires interdisciplinary treatment. However, it is difficult to predict its success.
Despite attenuated packing of GDCs, including eight fibered coils among 16 standard coils placed in the left cavernous sinus and the intercavernous portion of the cavernous sinus, the CCF remained open because of multiple fistula openings at the wall on both sides of the cavernous sinus. Intracavernous septations and venous thrombosis, as in our case (which have been found frequently coexisting with CCF [12]), limited the filling of the cavernous sinus with coils via a single approach. In cases of intracavernous thrombosis, one would expect that fibered coils increase the local thrombosis, which obviously was not observed in the case reported herein. Likewise, low concentrated Ethibloc applied on the arterial and venous side did not induce intracavernous thrombosis. Furthermore, the transarterial embolization showed only marginal reduction of the shunt volume and multiple fistula points persisted.
Because the neurologic symptoms did not improve, a third session was indicated to prevent visual loss. Bilateral fistulae do not necessarily require bilateral treatment. Bilateral SOV treatment was described as being performed in one patient in one session (9) and in one patient in two sessions (8). After repeatedly failing to reach the left side of the cavernous sinus via the right SOV approach, we had to choose the SOV approach via the left side despite the present thrombosis. Until now, the approach through a thrombosed SOV had been described in only two cases (8). This left SOV approach resulted in complete occlusion with GDCs and an almost complete recovery within 6 weeks. This case and both previously described cases (8) show that it is technically possible, although it may be associated with a higher rate of complications because of difficulties in identifying the SOV intraoperatively. Furthermore, in cases with CCF and failed embolization via several transvenous approaches, an earlier interdisciplinary decision to use the safe, direct, and efficient SOV approach should be made, even if the SOV is thrombosed.
References
- Received April 14, 2002.
- Accepted after revision June 7, 2002.
- Copyright © American Society of Neuroradiology